
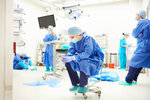

There has been much in the news about healthcare worker burnout. Burnout has resulted in crisis-level losses of staff and expertise since before COVID-19, which the pandemic exacerbated. Addressing burnout is as important as training more workers. Lost seasoned professionals take years of experience and wisdom, gleaned from time in the field, when they leave. This cannot be quickly replicated in the newly trained.
I suggest you read this column from a personal – as well as societal and healthcare impact – perspective. How are you, your loved ones, and your friends doing in your jobs?
I experience burnout in transactional (vs interactional) healthcare visits and poor customer service in commercial interactions. Burnout affects and is a problem in all aspects of society.
The World Health Organization (WHO) classifies burnout as a “syndrome conceptualized as resulting from chronic workplace stress that has not been successfully managed.” Its three main symptoms are:
The WHO describes burnout as an occupational phenomenon, not a medical condition. That said, burnout is a kind of depression of the ‘work soul’ and can lead to medical conditions including depression, anxiety, substance abuse, and overeating. It can result in wanting to quit (and leaving) one’s job.
(from the Harvard Business Review):
6 Causes of Burnout, and How to Avoid Them (hbr.org)
Burnout is not just being tired. It is a condition that requires interventions: prevention and treatment interventions by employers and self-care by employees.
The current data on healthcare workers corroborate this list of the causes of burnout from business research. In addition, healthcare workers deal with unique stresses that include taxing work (long and non-traditional shifts that need to be filled 25/7/365) as well as significant safety risks. Safety risks entail exposure to infectious diseases, long and often unpredictable hours, as well as stressful interactions with patients and families who have become increasingly threatening and at times violent.
No longer working on the front lines of healthcare, I was shocked to hear from an ER RN colleague from Milwaukie, WI, that he experiences at least three threats to his life on EVERY ER shift! Reading Edwin Leap M.D.’s column (www.edwinleap.com) confirms this and I have no doubt these risks exist locally. An RN friend from Bremerton shared that during the pandemic, she and staff were incessantly harassed and blamed for causing patients to be ill with COVID-19 (despite their attending a party to get exposed) rather than being thanked for caring for them.
Medscape publishes online updates on medicine and performs studies on physicians’ work lives. A review on burnout in internists showed up this week and caught my attention.
Internal Medicine physicians, like me, are also called internists (different from interns who are first-year doctor trainees). Yup, confusing. Internists now mostly work as hospitalists. They are primary care physicians for those who are hospitalized. Sadly, internists rarely practice outpatient primary care these days.
The news about internist burnout is grim.
Half of US internists experienced burnout last year. The main causes? Lack of autonomy over their practices, plus the burden of bureaucratic tasks and paperwork over which they feel no control. As a result, half of them have considered leaving medicine. Amid a critical primary care physician shortage, this is very bad news.
The news is not better for other healthcare professionals.
In November 2023, the CDC published a paper in the MMWR (Morbidity and Mortality Report, a weekly update on what is happening in healthcare) called
In 2022, nearly half of healthcare workers reported feeling burnt out often. 44% reported they were likely to look for a new job, called ‘turnover intention.’ This compares to 14% in fields other than healthcare. It also showed that US healthcare workers experienced greater declines in mental health, job, and life satisfaction than other workers.
In this time of severe healthcare workforce shortages, this too is very bad news.
Because preventing burnout is good for all of us and our society to prosper.
The Surgeon General’s report states that distressing work environments contributed to a record-high number of healthcare workers quitting their jobs. “These data support an imperative call to action to create a system where healthcare workers can thrive.”
The report also called out the importance of ‘decent work’ in our society (safe work that provides a fair income and opportunities for growth and productivity) as a public health goal…that is, for everyone.
Optimistically, the Surgeon General’s report notes that modifiable working conditions can make all the difference, and much more quickly than training new healthcare professionals. Preventing burnout is a potent solution for maintaining staff.
The National Institute for Occupational Safety and Health (NIOSH) has responded to this problem with a robust tool called Impact Wellbeing. In this 100+ page document are buckets of strategies for organizations to use to prioritize professional well-being.
The introduction states, “Positive and safe working conditions, including trust in management and supervisor help, were associated with lower odds of burnout in staff. “This tool offers evidence-based solutions to hospitals to reduce burnout, sustain staff well-being, and build a system where healthcare workers thrive.”
*See column A caring difference you can feel, Dec 26, 2023, on how one Washington community hospital’s leadership is well on its way to incorporating these tools.
The complexity of corporatized hospital organizations has slowed their implementation of such burnout prevention strategies. It is hoped that they will buy in as soon as possible as these entities control a majority of healthcare in our state.
I believe that what is good for patient- care and healthcare professionals is important for healthcare organizations’ success in providing care to their communities. Burnout, loss of expertise, staff turnover, and re-training are time-consuming, expensive, and impair quality of care, morale, and trust.
Keeping current staff working is a powerful way to reduce staff shortages and brain drain.
If you are experiencing burnout, here’s what you can do:
6 Causes of Burnout, and How to Avoid Them (hbr.org) This short article has excellent and practical suggestions on what to do if you are experiencing burnout.
Reducing worker burnout is a foundational solution to the healthcare worker shortage. Let’s keep our doctors and nurses and all their support staff on the job!
P.S. I am interested to hear from readers, our local healthcare workers, and leaders in response to these columns using your input for more columns on these important topics!
Debra L. Glasser, M.D., is a retired internal medicine physician in Olympia. Got a question for her? Write drdebra@theJOLTnews.com
4 comments on this item Please log in to comment by clicking here
mtndancer
Is there any one of these burnout issues that does not eventually lead back to investors squeezing every possible dollar out of our health care (non)system?
Tuesday, April 23 Report this
Chappellg
I agree with mtndancer.. even our nonprofits are squeezing every dollar out, closing unprofitable departments, understaffing, overworking everyone in the corporation—all to the detriment of the employees and the patients
Wednesday, April 24 Report this
KellyOReilly
Dear Debra, thank you for yet another thorough and well-written article regarding the ills of our HC system! Thank you for informing us that most internists now work only in hospitals. This helps to explain why finding a primary care physician has been so difficult, not that it's ever been easy! Nonetheless, I will continue my search for a PCP and I am attempting to educate myself on how to navigate the HC system. Your articles are valuable in this regard and I appreciate the time and effort you put into them! I've just purchased a new book on navigating the HC system from the perspective of women of color by Sharon Malone, MD: "Grown Woman Talk: Your Guide to Getting and Staying Healthy". Although I'm not a person of color, I've not appreciated the way in which some HC providers fail to take we ladies seriously. Thank you for clearly defining professional burnout in this article. So many of us can relate to this condition, myself included. Although my career was not in HC, I was extremely burnt out at the end of my career and I thank Heaven to be retired! I read you 12/26/23 too; and it's good to know that there is hope that positive change can happen when people put there minds to it.
Wednesday, April 24 Report this
EKershisnik
Because the term "Burnout" may unintentionally suggest a deficiency or shortcoming of the clinician who is suffering, an alternative term, "Moral Injury" has been proposed. You alluded to this in acknowledging the role of systemic pressures from corporations. Moral injury describes the challenge of simultaneously knowing what care patients need but being unable to provide it due to constraints that are beyond our control.
Wednesday, April 24 Report this